CASE HISTORY
A term, appropriate-for-gestational-age neonate with normal APGAR scores and no history of perinatal hypoxia presented with seizures on day 2 of life. There were no antenatal or perinatal complications. Initial consideration was hypoxic–ischemic encephalopathy (HIE); however, the clinical history was discordant with this diagnosis.
CASE CONTRIBUTED BY
Dr Thapasya, DNB resident, KMCH, Coimbatore
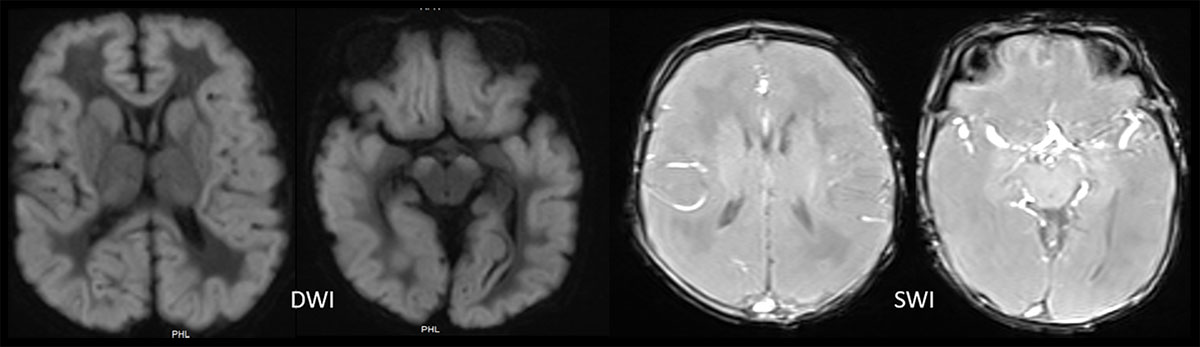
DWI: Diffuse, symmetric cortical thickening with widespread diffusion restriction, involving bilateral cortical and subcortical regions, basal ganglia, thalami, and cerebral peduncles.
SWI: Susceptibility-weighted imaging shows no hemorrhage
MRI Spectrum
Acute: Diffuse white matter and caudate T2 hyperintensity with widespread diffusion restriction; MRS shows elevated lactate and reduced NAA.
Subacute: T1/T2 shortening of basal ganglia, mimicking HIE, with relative thalamic sparing.
Chronic: Severe volume loss of basal ganglia and white matter with cystic degeneration.
Imaging Differentials:
HIE-like metabolic disorders (MoCD/ISOD)
Epileptic encephalopathy
Mitochondrial cytopathy.
Diagnosis: Targeted metabolic evaluation followed by genetic testing confirmed molybdenum cofactor deficiency.
LIKELY COMPOUND HETEROZYGOUS VARIANTS TO BE CAUSATIVE OF THE REPORTED PHENOTYPE WERE IDENTIFIED
| Gene (Transcript) | Location | Variant | Zygosity | Disease (OMIM) | Inheritance | Classification |
| MOCSI (-) (ENST00000373186.4) | Exon 7 | c.955C>T (p.Arg319Ter) | Heterozygous | Molybdenum colactor deficiency of complementation group A | Autosomal recessive | Pathogenic |
| Exon 1 | c.217C>T (p.Arg73Trp) | Heterozygous | Likely Pathogenic |
“Reclassification of these variants could be considered based on parental testing.”
Discussion:
Hypoxic–ischemic encephalopathy (HIE) is the most common cause of neonatal encephalopathy. MoCD leads to toxic sulfite accumulation, resulting in severe excitotoxic neuronal injury and HIE-like imaging patterns, often in the absence of a hypoxic insult.
Conclusion:
MoCD is a HIE-like imaging patterns that are discordant with clinical history, thucritical metabolic mimic of HIE. Imaging plays a pivotal role in identifying molybdenum cofactor deficiency by recognizing s guiding timely metabolic and genetic testing, preventing misdiagnosis.
| Feature | HIE | MOCD |
| Perinatal hypoxia | Present | Absent |
| DWI pattern | Watershed/deep nuclei | Diffuse, non-vascular |
| Brainstem (cerebral peduncles) | Spared | Involved (hallmark) |
| SWI microbleeds | Rare | Absent |
| Evolution | Cystic encephalomalacia | Rapid atrophy, no cysts |
| MRS | ↑Lactate | ↓↓NAA, ↑Lactate, ↑Glutamine |

Add a Comment
You must be logged in to post a comment